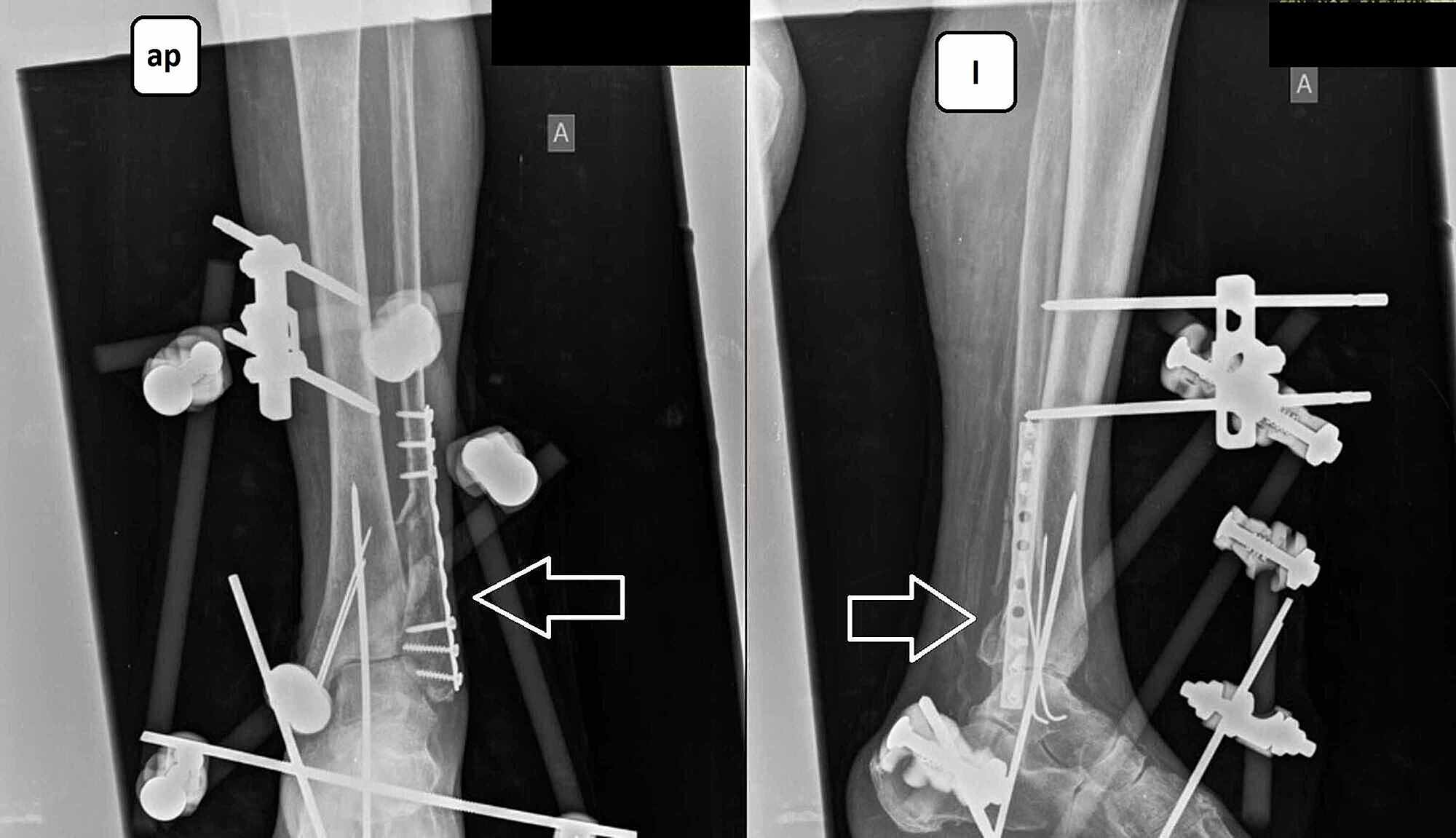
In this case, a large osteochondral fragment of the patella was easily visualized and removed. Loose bodies may be removed arthroscopically by enlarging the medial portal and then may be kept on the sterile back table. It is imperative to visualize the medial and lateral gutters, as osteochondral fragments and loose bodies often are found in these locations. After standard skin preparation and draping, a diagnostic arthroscopy is performed to assess the extent of the injury and any other concomitant intra-articular injuries. The patient is positioned supine with or without a nonsterile tourniquet applied, as per surgeon preference. 
12 Small, bioabsorbable screws have been shown to be appropriate viable and alternative option for osteochondral fixation, as they afford both strong compression and fixation strength with the need for later surgical removal lessened. 8, 13 Suture-only techniques provide adequate strength with minimal prominence but do not create compression across the fracture fixation. Metal screws can afford excellent fixation strength and compression but risk creating a new fracture and also can become prominent, requiring a second surgery for later removal. 7, 8, 9, 10, 11, 12 The choice of implant and technique is surgeon-specific, with each technique having relative risks and benefits. Various fixation methods have been described, ranging from metal screw fixation to suture-only bridging techniques. 2, 6 Adequate internal fixation is necessary to allow early joint mobilization while preventing further chondral surface damage and early joint degeneration. Larger chondral and osteochondral fragments should be managed with surgical fixation. Small cartilage fragments (<5 mm) may be treated with removal and debridement, as they may enlarge over time or become abrasive loose bodies. 2, 3, 4 Although many isolated patellar dislocations may be managed nonoperatively, the presence of an osteochondral fracture or an osteochondral loose body is an indication for prompt surgical intervention. 5, 6 For this reason, many authors recommend obtaining further imaging (magnetic resonance imaging or computed tomography) after an initial traumatic injury episode to ensure there are no osteochondral injuries and/or loose fragments present within the joint. 2 Large osteochondral fragments or bony defects may be visualized on standard radiographs, but often the fragments may only contain a small bony portion and thus, are typically best visualized by using magnetic resonance imaging or computed tomography. Historically, first-time patellar dislocations were managed nonoperatively without any further imaging beyond plain radiographs. 5 Standard anteroposterior, lateral, and merchant or sunrise radiographs should be obtained during the initial evaluation. 3 Associated injuries include medial patellofemoral ligament tears, bone contusions, and/or impaction injuries to the lateral femoral condyle. In the acute setting, patients often present with a large knee effusion and tenderness over the medial retinaculum. 4, 5, 6 Early recognition and treatment is vital to maintaining chondrocyte viability and restoring the articular congruity of the patella. 2 These injuries are most common in children and adolescents, often in the setting of an unstable osteochondritis dissecans lesion, but can occur after a traumatic injury in the adult population as well. The most common site of osteochondral fracture or isolated chondral injury is the medial facet of the patella, followed by the central facet of the patella, and finally the lateral femoral condyle. 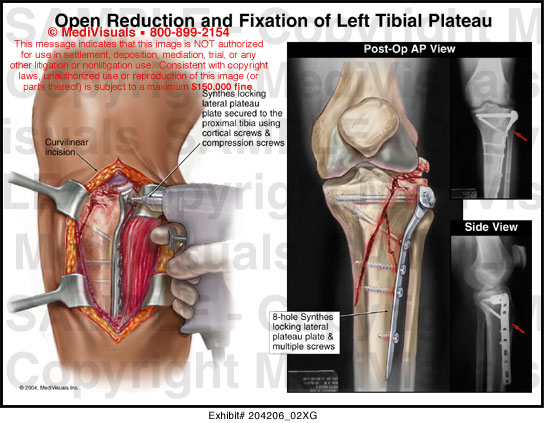
1, 2, 3 The dislocation can result in a small, shearing injury to the chondral surface alone or can result in a large osteochondral fracture fragment. Osteochondral injuries after a single lateral patellar dislocation have been reported to occur in between 38% and 95% of cases.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
